Skip NavigationSkip to Primary Content

Specialty Services

Internal Medicine
Our internal medicine service provides examinations, diagnostic tests, and a wide variety of therapies to help your sick dogs and cats get better.

Feline Radioiodine Treatment
Feline Hyperthyroidism is the most common endocrine disease seen in cats. OVSH offers diagnostics and treatments to help your cat recover.
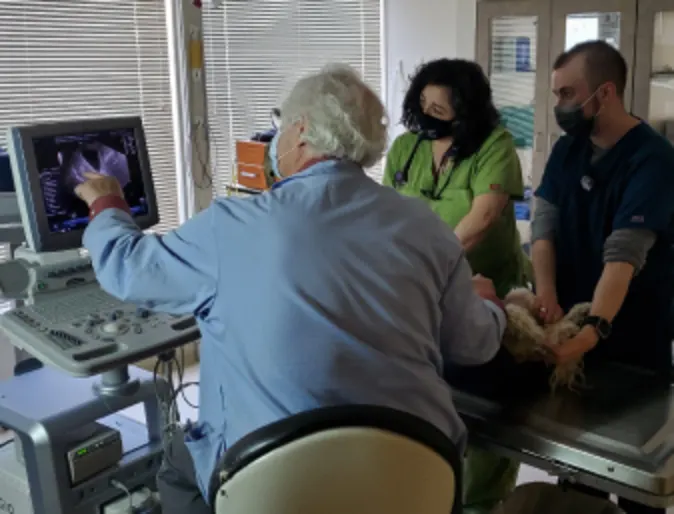
Diagnostic Ultrasounds
We offer diagnostic ultrasounds to evaluate heart conditions, internal organs, cysts and tumors, and more during your visit at OVSH.

Beaverton's Specialty Veterinarian
At Oregon Veterinary Specialty Center, some of our treatments and services include:
Internal Medicine
Oncology
CT Imaging
Therapeutic Laser Treatment
Dr. Franklin is board certified by the American College of Veterinary Internal Medicine. Our knowledgeable and friendly staff will be happy to answer your questions about our care and services. Schedule an appointment today.
Client Reviews and Testimonials
Our staff at Veterinary Services values feedback from our clients. Here is just a small sample of the hundreds of happy and healthy pets that we have cared for since 1979.
